"ECPs can be trained in 2 years, whereas it would take nearly a decade and…
Education that saves lives
By: Rashidah Nambaziira, GECC Program Coordinator – Masaka
“The ECPs have proved that training non-physician clinicians in Emergency Medicine can go a long way in improving management of critical patient care within an existing low resource system.”
GECC started training nurses to provide Emergency Care in Nyakibale Hospital, and has recently started a similar program at Masaka Regional Referral Hospital (MRRH). For the past 12 months, nurses have run the MRRH Emergency Department under the supervision of GECC Qualified Emergency Care Providers (ECPs).
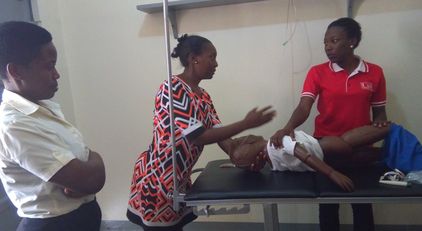
A month ago, a 10-year-old girl was brought into the ED, referred from Nkozi private hospital with a tib/fib fracture, and abdominal pain following a fall off of a motorcycle. Teddy, a qualified ECP, together with a student nurse triaged the patient as priority, assessed her, mobilized her fracture, started IV fluids, and blood work to get blood for the patient. Teddy also did a bedside ultrasound and diagnosed internal bleeding; the patient needed blood transfusion, and emergency laparotomy. MRRH has a functional lab, a general surgeon, and a blood bank, but the patient couldn’t get the blood or the laparotomy because the hospital had no blood. The patient was referred to a private hospital, Kitovu, for further management, and Teddy went on to see another critical patient.
 MRRH provides free healthcare to the sickest patients referred in from clinics, private hospitals, and other health facilities in 7 surrounding districts, but like other government hospitals, it frequently stocks out of essential supplies like blood, oxygen, some antibiotics, etc. Additionally, certain specialists/ special units (burn unit, ICUs, heart institutes), and certain investigations (CT scans, endoscopy, biopsy) are only available at the National Referral Hospital, or International Hospitals. Furthermore, MRRH, like other government hospitals, is extremely understaffed for the overwhelming numbers and severity of patients they see; 7 doctors (only 3 of these are specialists) and at most 2 nurses per shift per ward, attending to thousands of patients in 14 wards, including the Emergency Department, which receives the sickest patients in the region.
MRRH provides free healthcare to the sickest patients referred in from clinics, private hospitals, and other health facilities in 7 surrounding districts, but like other government hospitals, it frequently stocks out of essential supplies like blood, oxygen, some antibiotics, etc. Additionally, certain specialists/ special units (burn unit, ICUs, heart institutes), and certain investigations (CT scans, endoscopy, biopsy) are only available at the National Referral Hospital, or International Hospitals. Furthermore, MRRH, like other government hospitals, is extremely understaffed for the overwhelming numbers and severity of patients they see; 7 doctors (only 3 of these are specialists) and at most 2 nurses per shift per ward, attending to thousands of patients in 14 wards, including the Emergency Department, which receives the sickest patients in the region.When the 10-year-old girl came in, there were 3 qualified ECPs in the ED. She was stabilized and referred to the right facility in the shortest time possible. Meanwhile, the other 2 ECPs attended to similarly critical patients. With one regular nurse and one doctor, who’s not emergency trained, the girl would have had to wait in line, with her plummeting HB levels, for a more critical patient to be seen first.
Since the arrival of ECPs, the efficiency in managing critical patients in the MRRH ED has improved: the 4 ECPs in the ED are all comprehensively trained to independently assess and stabilize patients, so more patients are seen at once. With additional skills like bedside Ultrasound and Imaging interpretation, the ECPs diagnose critical conditions, stabilize the patient, and call the necessary specialist, or refer the patient to a better-equipped facility in the shortest time possible.
In a low resource setting like MRRH, referrals are inevitable and necessary; the important thing is to recognize the patient’s critical condition, provide the best emergency care to stabilize them, and get them to a more equipped facility in the shortest time possible. For the past 12 months, the ECPs have done just that, and have proved that training non-physician clinicians in Emergency Medicine can go a long way in improving management of critical patient care within an existing low resource system.


This Post Has 0 Comments